Investigating resistance in clinical Mycobacterium tuberculosis complex isolates with genomic and phenotypic antimicrobial susceptibility testing: a multicentre observational study
Publicacion con colaboración de nuestros investigadores Eduardo Gotuzzo y Tatiana Cáceres
Iris Finci*, Audrey Albertini*, Matthias Merker*, Sönke Andres, Nino Bablishvili, Ivan Barilar, Tatiana Cáceres, Valeriu Crudu, Eduardo Gotuzzo, Nchimunya Hapeela, Harald Hoffmann, Christine Hoogland, Thomas A Kohl, Katharina Kranzer, Anna Mantsoki, Florian P Maurer, Mark P Nicol, Ecaterina Noroc, Sara Plesnik, Timothy Rodwell, Morten Ruhwald, Theresa Savidge, Max Salfinger, Elizabeth Streicher, Nestani Tukvadze, Robin Warren, Widaad Zemanay, Anna Zurek, Stefan Niemann†, Claudia M Denkinger†
*Joint first authors who contributed equally †Joint last authors who contributed equally
Abstract
Background: Whole-genome sequencing (WGS) of Mycobacterium tuberculosis complex has become an important tool in diagnosis and management of drug-resistant tuberculosis. However, data correlating resistance genotype with quantitative phenotypic antimicrobial susceptibility testing (AST) are scarce.
Methods: In a prospective multicentre observational study, 900 clinical M tuberculosis complex isolates were collected from adults with drug-resistant tuberculosis in five high-endemic tuberculosis settings around the world (Georgia, Moldova, Peru, South Africa, and Viet Nam) between Dec 5, 2014, and Dec 12, 2017. Minimum inhibitory concentrations (MICs) and resulting binary phenotypic AST results for up to nine antituberculosis drugs were determined and correlated with resistance-conferring mutations identified by WGS.
Findings: Considering WHO-endorsed critical concentrations as reference, WGS had high accuracy for prediction of resistance to isoniazid (sensitivity 98·8% [95% CI 98·5-99·0]; specificity 96·6% [95% CI 95·2-97·9]), levofloxacin (sensitivity 94·8% [93·3-97·6]; specificity 97·1% [96·7-97·6]), kanamycin (sensitivity 96·1% [95·4-96·8]; specificity 95·0% [94·4-95·7]), amikacin (sensitivity 97·2% [96·4-98·1]; specificity 98·6% [98·3-98·9]), and capreomycin (sensitivity 93·1% [90·0-96·3]; specificity 98·3% [98·0-98·7]). For rifampicin, pyrazinamide, and ethambutol, the specificity of resistance prediction was suboptimal (64·0% [61·0-67·1], 83·8% [81·0-86·5], and 40·1% [37·4-42·9], respectively). Specificity for rifampicin increased to 83·9% when borderline mutations with MICs overlapping with the critical concentration were excluded. Consequently, we highlighted mutations in M tuberculosis complex isolates that are often falsely identified as susceptible by phenotypic AST, and we identified potential novel resistance-conferring mutations.
Interpretation: The combined analysis of mutations and quantitative phenotypes shows the potential of WGS to produce a refined interpretation of resistance, which is needed for individualised therapy, and eventually could allow differential drug dosing. However, variability of data for some M tuberculosis complex isolates carrying identical mutations also reveals limitations of our understanding of the genotype and phenotype relationships (eg, including epistasis and strain genetic background).
Funding: Bill & Melinda Gates Foundation, German Centre for Infection Research, German Research Foundation, Excellence Cluster Precision Medicine of Inflammation (EXC 2167), and Leibniz ScienceCampus EvoLUNG.
Copyright © 2022 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license. Published by Elsevier Ltd.. All rights reserved.

![Abstract Background: Whole-genome sequencing (WGS) of Mycobacterium tuberculosis complex has become an important tool in diagnosis and management of drug-resistant tuberculosis. However, data correlating resistance genotype with quantitative phenotypic antimicrobial susceptibility testing (AST) are scarce. Methods: In a prospective multicentre observational study, 900 clinical M tuberculosis complex isolates were collected from adults with drug-resistant tuberculosis in five high-endemic tuberculosis settings around the world (Georgia, Moldova, Peru, South Africa, and Viet Nam) between Dec 5, 2014, and Dec 12, 2017. Minimum inhibitory concentrations (MICs) and resulting binary phenotypic AST results for up to nine antituberculosis drugs were determined and correlated with resistance-conferring mutations identified by WGS. Findings: Considering WHO-endorsed critical concentrations as reference, WGS had high accuracy for prediction of resistance to isoniazid (sensitivity 98·8% [95% CI 98·5-99·0]; specificity 96·6% [95% CI 95·2-97·9]), levofloxacin (sensitivity 94·8% [93·3-97·6]; specificity 97·1% [96·7-97·6]), kanamycin (sensitivity 96·1% [95·4-96·8]; specificity 95·0% [94·4-95·7]), amikacin (sensitivity 97·2% [96·4-98·1]; specificity 98·6% [98·3-98·9]), and capreomycin (sensitivity 93·1% [90·0-96·3]; specificity 98·3% [98·0-98·7]). For rifampicin, pyrazinamide, and ethambutol, the specificity of resistance prediction was suboptimal (64·0% [61·0-67·1], 83·8% [81·0-86·5], and 40·1% [37·4-42·9], respectively). Specificity for rifampicin increased to 83·9% when borderline mutations with MICs overlapping with the critical concentration were excluded. Consequently, we highlighted mutations in M tuberculosis complex isolates that are often falsely identified as susceptible by phenotypic AST, and we identified potential novel resistance-conferring mutations. Interpretation: The combined analysis of mutations and quantitative phenotypes shows the potential of WGS to produce a refined interpretation of resistance, which is needed for individualised therapy, and eventually could allow differential drug dosing. However, variability of MIC data for some M tuberculosis complex isolates carrying identical mutations also reveals limitations of our understanding of the genotype and phenotype relationships (eg, including epistasis and strain genetic background). Funding: Bill & Melinda Gates Foundation, German Centre for Infection Research, German Research Foundation, Excellence Cluster Precision Medicine of Inflammation (EXC 2167), and Leibniz ScienceCampus EvoLUNG. Copyright © 2022 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license. Published by Elsevier Ltd.. All rights reserved. Abstract Background: Whole-genome sequencing (WGS) of Mycobacterium tuberculosis complex has become an important tool in diagnosis and management of drug-resistant tuberculosis. However, data correlating resistance genotype with quantitative phenotypic antimicrobial susceptibility testing (AST) are scarce. Methods: In a prospective multicentre observational study, 900 clinical M tuberculosis complex isolates were collected from adults with drug-resistant tuberculosis in five high-endemic tuberculosis settings around the world (Georgia, Moldova, Peru, South Africa, and Viet Nam) between Dec 5, 2014, and Dec 12, 2017. Minimum inhibitory concentrations (MICs) and resulting binary phenotypic AST results for up to nine antituberculosis drugs were determined and correlated with resistance-conferring mutations identified by WGS. Findings: Considering WHO-endorsed critical concentrations as reference, WGS had high accuracy for prediction of resistance to isoniazid (sensitivity 98·8% [95% CI 98·5-99·0]; specificity 96·6% [95% CI 95·2-97·9]), levofloxacin (sensitivity 94·8% [93·3-97·6]; specificity 97·1% [96·7-97·6]), kanamycin (sensitivity 96·1% [95·4-96·8]; specificity 95·0% [94·4-95·7]), amikacin (sensitivity 97·2% [96·4-98·1]; specificity 98·6% [98·3-98·9]), and capreomycin (sensitivity 93·1% [90·0-96·3]; specificity 98·3% [98·0-98·7]). For rifampicin, pyrazinamide, and ethambutol, the specificity of resistance prediction was suboptimal (64·0% [61·0-67·1], 83·8% [81·0-86·5], and 40·1% [37·4-42·9], respectively). Specificity for rifampicin increased to 83·9% when borderline mutations with MICs overlapping with the critical concentration were excluded. Consequently, we highlighted mutations in M tuberculosis complex isolates that are often falsely identified as susceptible by phenotypic AST, and we identified potential novel resistance-conferring mutations. Interpretation: The combined analysis of mutations and quantitative phenotypes shows the potential of WGS to produce a refined interpretation of resistance, which is needed for individualised therapy, and eventually could allow differential drug dosing. However, variability of MIC data for some M tuberculosis complex isolates carrying identical mutations also reveals limitations of our understanding of the genotype and phenotype relationships (eg, including epistasis and strain genetic background). Funding: Bill & Melinda Gates Foundation, German Centre for Infection Research, German Research Foundation, Excellence Cluster Precision Medicine of Inflammation (EXC 2167), and Leibniz ScienceCampus EvoLUNG. Copyright © 2022 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license. Published by Elsevier Ltd.. All rights reserved.](https://imtavh.cayetano.edu.pe/images/gr1.jpg)
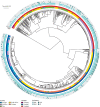
Phylogenetic relationship, origin, and individual drug resistances of 900 Mycobacterium tuberculosis complex isolates
The inner circle represents lineages. The circle in the middle represents origin countries of the samples. The outer circle consists of four lines with filled circles representing resistance to the following antibiotics: INH, RMP, SLID (kanamycin, capreomycin, or amikacin), and FQ (moxifloxacin or levofloxacin); order from inside towards outside. For both SLID and FQ, strains with resistance to at least one antibiotic were considered as resistant. INH=isoniazid. RMP=rifampicin. SLID=second-line injectable drugs. FQ=fluoroquinolones.





